International Awareness for Cancer
February 4th marks World Cancer Day, an initiative created by the Union for International Cancer Control (UICC) in 2000 to raise cancer awareness worldwide. This day is significant as it emphasises the immediate need to tackle the global burden of cancer. It unites people, communities, and nations in a call to action, raising awareness, promoting cancer education, and advocating for its research, prevention, detection, and treatment.
World Cancer Day 2024
Date: February 4, 2024
Why is World Cancer Day Important?
Cancer is the leading cause of death worldwide. And still, despite the surge of scientific and technological advancements in cancer prevention, diagnosis and treatment, the barriers to reaching cancer care have not diminished.
For a good reason, the World Cancer Day 2024 theme “Close the Care Gap” is very relevant.
Receiving cancer care should not be affected by education, income, or geographical location. Unfortunately, many patients encounter discrimination and prejudice based on ethnicity, gender, sexual orientation, age, disability and lifestyle, which may negatively affect the care they receive.
Addressing disparities in cancer care and ensuring equitable access to diagnosis, treatment, and palliative care is crucial to reducing the global cancer burden.
Current State of the Global Cancer Burden (2020)
By 2020, the world faced a significant challenge: there were around 19.3 million new cancer cases and nearly 10.0 million cancer deaths worldwide. Upon closer examination of the data, certain types of cancer became more prominent.
The most frequently diagnosed cancer during this period was breast cancer in women, with 12,5 % of all cancers, and it is estimated to be the most diagnosed tumour type among all cancer types and the leading cause of cancer death among women. Unfortunately, the incidence rates are increasing due to an urban lifestyle.
Lung cancer is the second most diagnosed cancer, with 12,2 % of all cancer types, and the leading cause of cancer death in men and second one for women. However, in many EU countries, the incidence rates have been declining, a trend that has been attributed to smoking prevention policies.
Colorectal cancer is the third most diagnosed cancer, with 10,7 % of all cancer types, the second cause of cancer death in men, and the third cause of cancer death in women. Although the incidence of colorectal cancer is increasing, earlier detection and more effective treatment have led to a decrease in mortality rates.
Prostate cancer is the most frequently occurring cancer in men, diagnosed in 7,8 % of all cancer types, and the third cause of cancer death in men. In recent years, the incidence and mortality rates have decreased in many EU countries.
Stomach cancer is the fifth most diagnosed cancer, with 6,0 % of all cancer types, and the estimated incidence in men was almost double that of women. The variability can be partly explained by various risk factors such as Helicobacter pylori infection, lifestyle choices (including smoking and alcohol consumption), salt intake, consumption of red meat, and genetic factors.
Projected Surge by 2040
It is estimated that the number of new cancer cases annually will rise to 28.4 million by 2040, indicating a significant escalation of the global burden of cancer in the coming years. This shows a substantial rise in the worldwide burden of cancer in the upcoming years, with a 47% increase from the 2020 figures. The surge of escalation is more evident in countries undergoing transition, with an increase ranging from 64% to 95%.
In contrast, transitioned countries might experience a rise of 32% to 56% in cancer cases. These projections are primarily driven by demographic shifts such as population growth and ageing. Additionally, increasing globalisation and economic development may further amplify these figures, emphasising the need for robust cancer control measures, especially in transitioning nations.
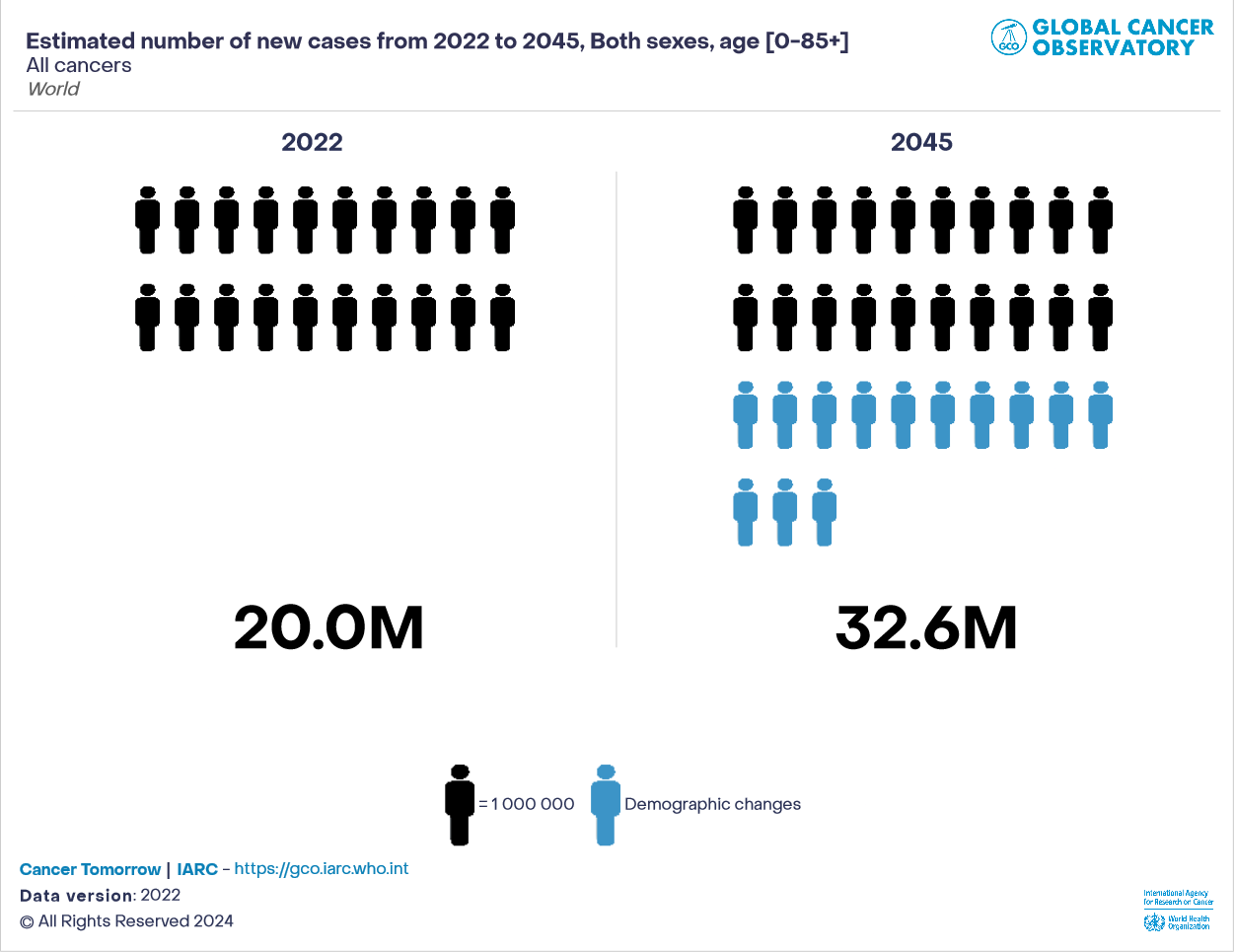
The Escalating Global Cancer Burden 2020-2040: Data visualisation courtesy of Global Cancer Observatory.
Why do Cancer Survival Rates Vary from Country to Country?
Survival rates of cancer patients can vary across different countries due to a variety of factors. The differences in healthcare systems between countries and the inequalities in healthcare access within countries can significantly impact these survival rates. It is generally observed that lower-income countries have lower survival rates for cancer patients, although there is some variation even among high-income countries.
Some of the most common factors include the type of cancer diagnosed, the available treatment options, and the stage at which cancer is detected and treated. Typically, the earlier the cancer is diagnosed and treated, the better the chances of survival.
Over the last few decades, there have been significant improvements in screening programs and treatments for specific types of cancers.
Preventive Measures for Cancer Risk Reduction
Preventive strategies are crucial in reducing cancer risk. These include adopting a healthy lifestyle, regular screening and vaccinations, avoiding tobacco and excessive alcohol consumption, and staying protected from harmful UV radiation.
Global Estimates of Preventable and Treatable Cancer Deaths
A recent study in The Lancet Global Health provides a comprehensive analysis of preventable and treatable deaths from 36 cancers worldwide. It estimates that in 2020, of the total cancer burden, 68.0% of premature deaths (aged 30–69 years) were preventable, and 32.0% were treatable. The study emphasises the need for greater investments in risk factor reduction and vaccination to address premature cancer inequalities and improve health systems. This research underlines the importance of tailored programs for early diagnosis and screening linked to comprehensive treatment to reduce the global cancer burden effectively.
Latest Medical Technology and Medicine in Cancer Care
Globally, there have been remarkable advancements in medical technology and medicine for cancer care. Research and development in these areas are crucial in improving survival rates and the quality of life for cancer patients.
Emerging Technologies for Cancer
Emerging technologies are showing promise in early cancer detection, and they are hot topics in cancer research. New technologies and advances could revolutionize the future of cancer treatment. Innovative techniques in molecular biology, such as gene-editing tools and nanomedicine, have the potential to become crucial for the future of cancer treatment. Breakthroughs in computer science, including artificial intelligence and virtual reality, may also initiate new cancer treatments, ranging from early cancer detection to improved quality of life for all cancer patients.
Emerging diagnostic, prognostic and predictive technologies
The tumour microenvironment (TME) is the complex surrounding of a tumour, made up of non-cancerous cells, including immune cells, fibroblasts, blood vessels, signalling molecules, and the extracellular matrix (ECM). Recent studies show that the TME plays an active role in promoting cancer progression. Understanding the TME has led to the development of effective therapies to treat advanced cancer.
Preclinical models and emerging technologies are available to study the effects of the tumour microenvironment on cancer heterogeneity and drug resistance. The preclinical tumour models include 2D cell culture, organoids, 3D cell culture, and organ-on-a-chip. Emerging analysis methods include single-cell RNA sequencing, spatial transcriptomisy and proteomics, metabolomics, and artificial intelligence.
Emerging cancer therapies
Using high-energy charged particles in radiotherapy has developed into an advanced form of cancer treatment. This biomedical application of nuclear physics is especially useful as the toxicities to healthy tissue are much lower than conventional photon therapy. It is also effective for re-irradiation and treating radio-resistant tumours. Charged particles are the most advanced technology for clinically translating ultra-high dose rate (FLASH) radiotherapy.
Promising approaches for cancer immunotherapies that are currently being tested in clinical trials or in the process of being approved by the FDA.
Adoptive cell therapy, also called cellular immunotherapy, is a type of treatment that employs our immune system’s cells to fight cancer. Our immune system has the ability to identify and remove infected, damaged, and cancerous cells. Cellular immunotherapies utilize this natural ability and can be utilized in various ways.
Cancer vaccines belong to a type of immunotherapy that can teach the immune system to recognize and eliminate cancer cells by making them familiar with their appearance. Since cancer cells look like healthy cells, it can be hard for the immune system to identify them as threats, but cancer vaccines can bridge this gap. Additionally, each person’s tumour has unique antigens that differentiate it from others. Certain cancers stem from viral infections, and preventive vaccines can reduce the risk of developing them.
Researchers have recently discovered a method to identify specific targets present in patients’ tumours that can help distinguish cancer cells from their normal cells. By making use of this knowledge, therapeutic cancer vaccines can be developed to target these specific targets. In some cases, these targets are normal proteins that are produced at abnormally high levels by cancer cells.
This has significantly expanded drug development for protein targets beyond DNA- and RNA-based targets. Targeting HER2 is one of the most successful examples of protein targeting. By combining the small molecule HER2 kinase inhibitor tucatinib with the naked or non-conjugated monoclonal anti-HER2 antibody trastuzumab, the indications for this therapy have expanded.
Gene therapy is a treatment method that has gained significant attention recently. It involves introducing therapeutic genes to cancer cells or tissues to either slow down cancer growth or cause cell death. There are different strategies used in gene therapy, such as activating tumour suppressor genes, inhibiting oncogene activation, immunotherapy, antiangiogenic gene therapy, and suicide gene therapy.
One example is CRISPR-based gene editing, which is a revolutionary tool for genome editing that has the potential to transform the field of cancer research and therapy. It allows scientists to target and edit specific genetic mutations that cause the growth and spread of tumours, which has opened up new possibilities for developing more personalized and effective cancer treatments.
HIGHLIGHTS
Liquid biopsy: Blood samples can provide doctors with valuable information about a tumour. By analysing traces of cancer DNA in the blood, doctors can determine which treatments are most effective, eliminating the need for invasive surgical biopsies.
Precision Oncology: This approach tailors treatment based on the genetic makeup of an individual’s cancer, ensuring more effective and targeted therapies.
Immunotherapy: This treatment boosts the body’s immune system to fight cancer cells more effectively.
AI and Machine Learning: Machine learning, biopsy, next-gen sequencing, and digital pathology are increasingly used for early cancer detection, diagnosis, and personalised treatment. These technologies identify patient-specific biological targets for cancer treatment.
Robotic Surgery: Minimally invasive surgeries, aided by robotics, offer more precision in removing tumours, leading to better outcomes and quicker recovery times.
Nanotechnology: This innovative field is opening new frontiers in drug delivery systems, making treatments more effective and less toxic.
Conclusion
World Cancer Day 2024 is a reminder of the collective effort required to conquer cancer. It’s a day to celebrate progress in cancer care and a call to action to continue the fight against this global health challenge. Through continued research, innovation, and shared knowledge, we can look forward to a future where cancer is no longer a life-threatening disease.




